Iron, Oxygen, and the Edge Between Performance and Damage

At FITNESS SF, we talk about progressive overload, VO₂ max, strength adaptation, and recovery. This discussion is based on a 2023 systematic review examining how iron levels influence physical performance in athletes.
One of the quiet variables that determines whether your training actually translates into adaptation is iron status. Not because iron is trendy. Not because it’s a supplement to experiment with. But because iron sits at the center of oxygen transport and cellular energy production.
Why Iron Matters for Athletes
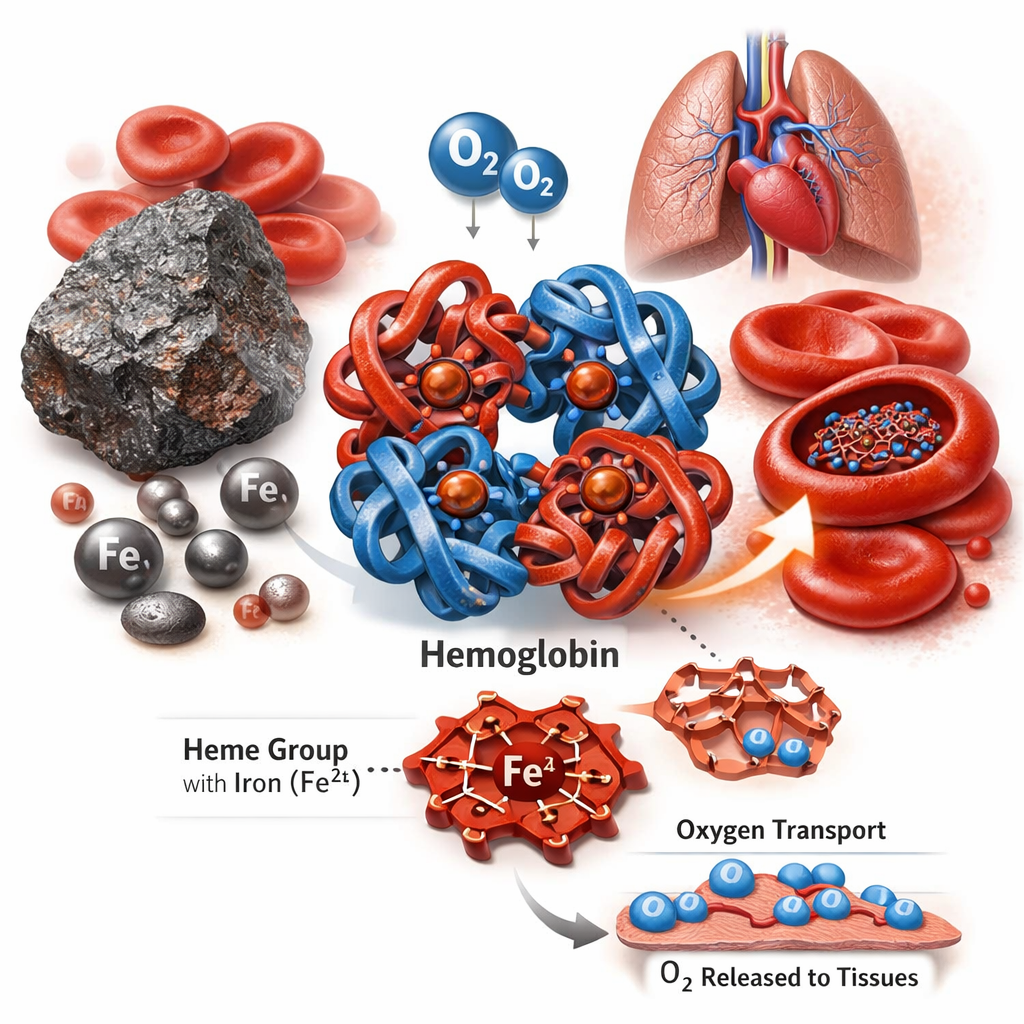
Iron allows hemoglobin to carry oxygen in the bloodstream. It allows myoglobin to shuttle oxygen inside muscle. It functions inside mitochondria where aerobic metabolism occurs.
When iron deficiency progresses to anemia, performance predictably declines. VO₂ max drops. Endurance capacity falls. Recovery worsens.
But here’s the nuance:
Even iron deficiency without anemia can impair performance. When ferritin (your iron storage marker) drops below roughly 20–30 ng/mL, studies consistently show that correcting the deficiency can improve markers like energetic efficiency, lactate response, and sometimes VO₂ max.
Above that threshold, supplementation becomes far less reliable as a performance tool.
Iron is not a booster.
It is a corrector.
Who Should Pay Attention?
Iron deficiency is most common in:
- Endurance athletes
- Female athletes
- High-volume training phases
- Calorie-restricted athletes
- Athletes training at altitude
Heavy training increases iron turnover and demand. Sweat, foot-strike hemolysis, GI microbleeding, and increased red blood cell production all contribute.
If you train hard and feel chronically fatigued despite disciplined programming, iron status deserves evaluation.
The Ferritin Question
Most labs define deficiency around:
Ferritin < 20–30 ng/mL
Performance improvements from supplementation are most consistent below this range.
What about higher levels?
There is no strong evidence that pushing ferritin from 60 to 110 ng/mL improves performance in otherwise healthy athletes training at sea level. In fact, once iron stores are sufficient, additional supplementation rarely increases hemoglobin or VO₂ max.
The goal is adequacy — not maximization.
Iron Is Powerful — and Potentially Harmful
Iron is highly redox-active. Its ability to donate and accept electrons makes it essential for life — and capable of causing damage.
Free iron can participate in Fenton reactions, generating reactive oxygen species that damage lipids, proteins, and DNA. This is why the body does not allow iron to circulate freely. It binds iron to transferrin in the blood and stores excess iron in ferritin.
There’s also an evolutionary layer here.
Pathogens require iron to replicate. In response to infection or chronic inflammation, the body increases production of hepcidin, a hormone that traps iron inside ferritin and reduces intestinal absorption. This process — often called “nutritional immunity” — is protective. The body hides iron from invaders.
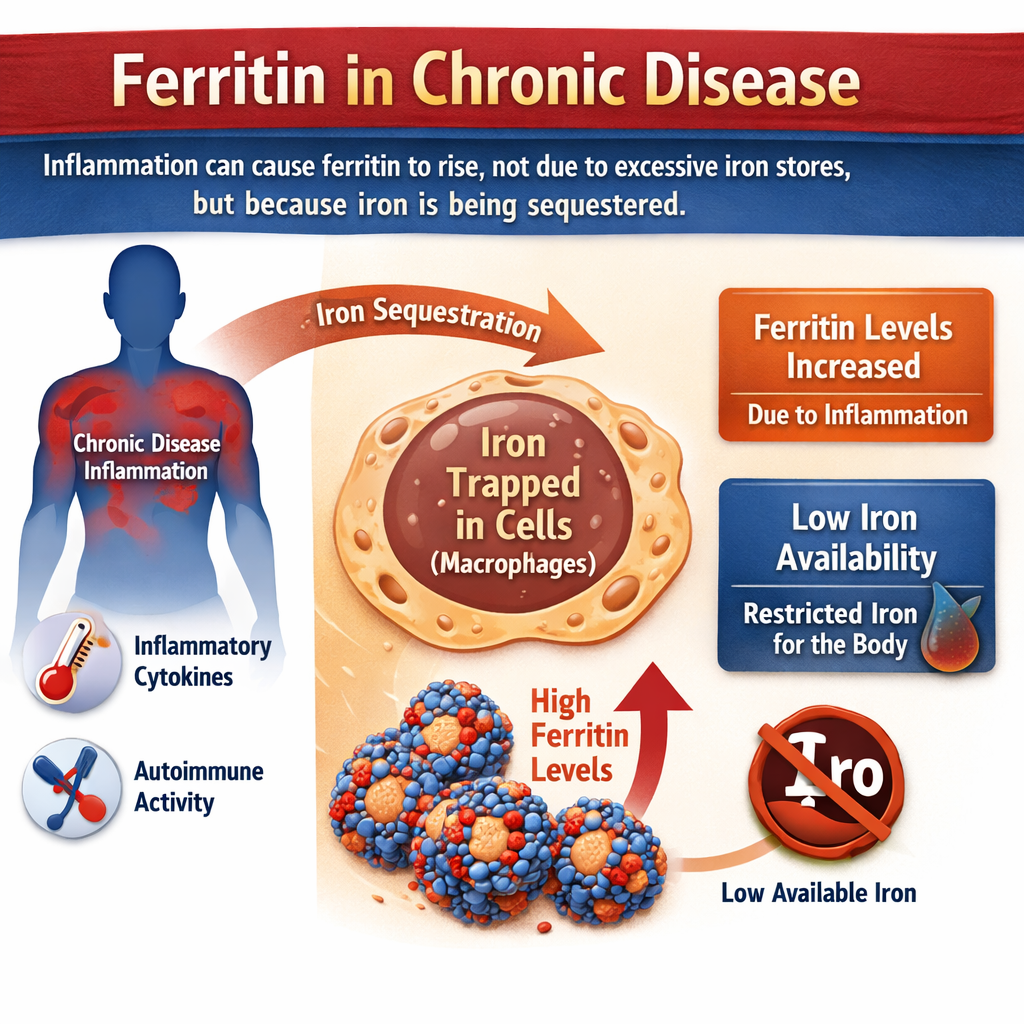
Iron regulation is sophisticated for a reason.
Too little impairs oxygen delivery.
Too much increases oxidative stress and tissue injury.
Training, Inflammation, and Hepcidin
After intense exercise, inflammatory signals rise. Hepcidin increases and peaks roughly three hours post-workout. During this window, iron absorption temporarily decreases.
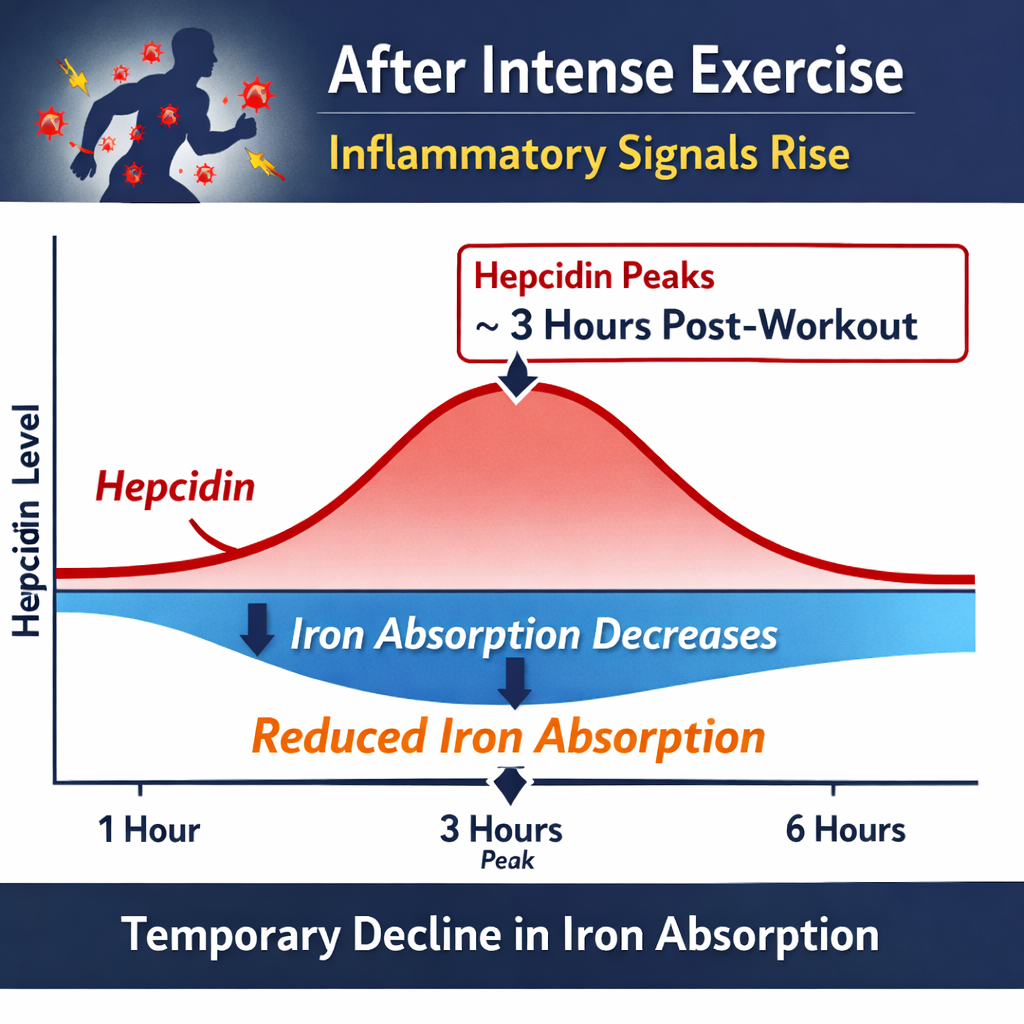
This means a few practical things:
- Chronic under-fueling may worsen iron regulation
- Low energy availability increases hepcidin
- Very low carbohydrate intake during heavy training can amplify stress signals
If you are training hard and chronically restricting calories, you may impair your ability to absorb iron — even if your intake is adequate.
Iron physiology does not operate in isolation from nutrition.
Altitude Changes the Rules
In hypoxic environments, erythropoietin rises. Red blood cell production accelerates. Iron demand increases.
Athletes with insufficient ferritin fail to optimally increase hemoglobin mass and VO₂ max at altitude. In this context, ensuring adequate iron stores before altitude exposure becomes critical.
But again — the goal is sufficiency, not overload.
Iron Doesn’t Work Alone
Two additional markers matter:
Vitamin D
Low vitamin D is associated with reduced hemoglobin and may influence erythropoietic signaling. Maintaining adequate levels supports overall oxygen transport.
Vitamin B12
B12 is required for red blood cell maturation. Inadequate B12 can impair hemoglobin synthesis even when iron is normal.
If you’re evaluating unexplained fatigue or performance decline, a broader view is smarter than focusing on ferritin alone.
Should You Supplement?
Here is the disciplined approach:
- Test first.
- Correct true deficiency.
- Reassess in 6–8 weeks.
Iron supplementation clearly benefits iron-deficient athletes.
In iron-sufficient athletes, performance gains are inconsistent. Excess supplementation may increase oxidative stress, elevate hepcidin, and in extreme cases contribute to iron overload.
Iron is not “more is better.”
It is “precisely regulated.”
The FITNESS SF Perspective
You can train brutally hard.
But if your oxygen delivery system is compromised — or if your micronutrient physiology is dysregulated — you will not adapt optimally.
At FITNESS SF, performance lives at the intersection of:
- Intelligent programming
- Adequate fueling
- Objective measurement
- Respect for physiology
Iron sits at that intersection.
If you are persistently fatigued, plateaued, or struggling to recover despite disciplined effort, it may be time to look beneath the surface.
Train with intention.
Recover with intelligence.
Build strength that lasts.


